Our scoping review resulted in 100 articles for data extraction and represented a range of examples where EL was used as an education strategy to prepare students from two or more disciplines for IPP. We provide a summary of final articles included from our scoping review in Supplementary file 3. We present the key findings from our review in three parts: 1) Part 1 provides an overall summary of descriptive elements of the included articles; 2) Part 2 provides the context of IPP education initiatives; and 3) Part 3 details the implementation and evaluation of IPP education initiatives. Given the total number of articles is 100, we report our findings in whole numbers that can be equated to percentage values.
Part 1: overall summary of articles
In this section we provide a description and background from the included literature that details the: 1) descriptive elements of the articles; 2) variation of terminology related to IPP in education; and 3) aim or purpose of the articles.
Descriptive elements of articles
The articles originated from 12 individual countries across four continents and described EL strategies for IPP education initiatives in three main typologies of literature – primary research, program description, and program evaluation (Fig. 3). The one article categorized as “other” was a practice guide focused on developing practice-based interprofessional learning [48]. Across those articles categorized as primary research and program evaluation, there was a range of methodological approaches used that included 25 quantitative, 25 mixed methods, 16 qualitative, and five case study designs (see Supplementary file # 2). Of note, there was one randomized control study [49] and five longitudinal studies identified [50,51,52,53,54].
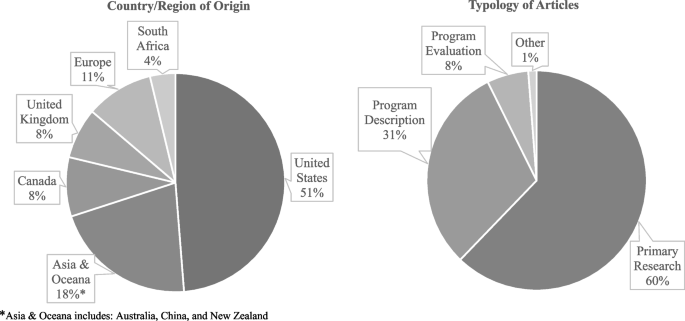
Articles by country/region of origin and typology of articles
Variation of terminology related to IPP in education
Our findings revealed that only two articles resulting from our search used IPP as the main concept in relation to IPP education initiatives in [55, 56], whereas the term interprofessional collaborative practice (IPCP) was used in five articles [50, 53, 57,58,59] and interprofessional education and collaborative practice was used in one article [60]. In 30 articles IPE was the sole concept used in association with IPP education initiatives. Interprofessional learning (IPL) was used in six articles [49, 61,62,63,64,65] and IPC in five articles [66,67,68,69,70] as synonymous terms for IPP. A range of other terms were used in conjunction with IPP including interprofessional learners [71], interprofessional (collaborative) service-learning [72,73,74,75,76], interprofessional training [77,78,79], interprofessional (clinical) placement [80,81,82], interprofessional clinic experience [83], interdisciplinary student placements [84], interdisciplinary student learning [55], interdisciplinary practice [85], interdisciplinary collaboration [86], interdisciplinary team or teamwork [87], integrated training [88], collaborative care training [89, 90], collaborative practice [88], interprofessional workplace [79], and interprofessional global service-learning [91].
Aim or purpose of the articles
The aim or purpose of the included articles was the explicitly stated or implied reason for why the paper was generated, which was often closely linked to the typology of the article (Fig. 3 and Supplementary file 2). Interpreting and reporting the typology of some articles posed a challenge as the aim or purpose was not explicitly stated [69, 70, 72, 91,92,93,94,95,96,97,98,99]. Where an explicit aim or purpose was not clear, a consensus how best to categorize the typology and describe the purpose was made by two or more members of our team from other information in the article. We identified three broad themes of purposes across the articles: a) describing and/or evaluating overall IPP initiative; b) evaluation of placements and experience on student outcomes; and c) experience, outcomes and/or impact of the IPP initiative on stakeholders (e.g., recipients of care, placement agencies, and collaborating partnerships). As some articles had more than one aim or purpose conveyed in the narrative or stated objectives these articles are represented in more than one theme.
-
a.
Describing and/or evaluating the overall IPP initiative. Fourty-four articles provided a description of planning, implementation and/or evaluation of elements of an IPP program [48,49,50, 57, 59, 60, 62, 65, 67, 69, 71, 72, 75, 78, 81, 87,88,89,90,91, 93, 96, 100,101,102,103,104,105,106,107,108,109,110,111,112,113,114,115,116,117,118,119,120,121], while the intent of one article was to describe the importance of IPP in relation to service delivery, care and meeting the needs of a population [122]. Program evaluation of the overall implementation or outcomes of an IPP initiative, such as curriculum design, was identified as a primary purpose in 13 articles [56, 59, 75, 95, 98, 114, 117, 123,124,125,126,127,128] and evaluation of impact of the IPP initiative on stakeholders (i.e., clients, health agency placements, etc.) was also identified [53, 59, 61, 62, 129]. Specifically introducing and/or evaluating the model, framework, or program design of the IPP initiative was a stated purpose [86, 118, 130, 131] and understanding processes of student learning through IPP curriculum design and experiences was also noted [132,133,134].
-
b.
Evaluation of placements and experience on student outcomes. Evaluation of the impact of clinical placements on students’ attitudes and/or perspectives towards IPE, IPC, IPL, IPP, and/or their placement experience was a purpose in 30 articles [49,50,51,52, 63, 65, 68, 72, 73, 76,77,78, 82, 83, 85, 98, 117, 118, 121, 122, 130, 135,136,137,138,139,140,141,142,143]. In 28 articles a purpose was to describe some specific aspect of the students’ perceptions on their experience, learning, or success from the IPP education initiative, such as competency development, cultural beliefs, interprofessional socialization, understanding of complex health issues, or other aspect of professional development [49,50,51, 54, 55, 58, 60, 66, 72, 74, 75, 79, 80, 97,98,99, 116, 118, 122, 123, 127, 130, 133, 142, 144,145,146,147]. Two articles evaluated student perspectives on their placement experience in relationship to their intentions to pursue a particular focus, such as working in primary care or rural settings [94, 139].
-
c.
Impact of the IPP initiative on stakeholders. The effect of IPP on client and service outcomes that included health status was a purpose in two articles [59, 62], while other articles aimed to evaluate experiences and perspectives of clients and their families on students engaged in IPP [50, 78, 84]. Six studies sought to assess the impact of the IPP initiative on clinical stakeholders and partnerships, such as effects of IPP on staff, collaboration or teamwork, practice efficiencies, and the health agency hosting placements [53, 59, 63, 64, 133, 148].
Part 2: context of IPP Education Initiatives
This part provides the context of IPP education initiatives described in the literature and includes: 1) a general overview of the initiatives; 2) the intention of experiential learning in the initiatives; 3) nature of student participation in the initiatives; 4) populations served by the initiative; and 5) involvement of instructional personnel and stakeholders.
General overview of IPP Education Initiatives
In Table 1 we present a summary of the student disciplines involved in IPP education initiatives, the various settings in which the initiatives were situated, and the types of services students engaged in as part of their learning experience.
Intention of experiential learning in IPP education initiatives
The intention of the EL IPP education initiatives was either explicitly stated or described by authors as the rationale for designing and implementing the initiative. Similar to our findings for purpose, several articles appeared to have more than one intention for the IPP initiative. In 22 articles, creation of learning initiatives for planned and/or authentic placements and experiences for interprofessional experiences was an intention of the IPP education initiative [51, 58, 62, 64, 67, 76, 78, 81, 85, 89, 95, 101, 103,104,105, 107, 117, 118, 120, 134, 139, 148]. Related to this, 20 of the initiatives were designed to build on IPE, IPL, and/or IPC theory or experiences through the initiative [48, 59, 70, 80, 87, 92, 106, 109, 111, 112, 114, 128, 131, 133, 135, 137, 138, 140, 141, 144]. Gaining familiarity with other disciplines and professions and learning from each other was cited as an intention in 16 of the IPP education initiatives [55, 56, 64, 65, 73, 74, 82, 88, 91, 98, 115, 121, 130, 134, 135, 141]. For 10 of the articles an intent was to provide IPP EL to pairings of specific student disciplines, such as: medicine and pharmacy [68, 121]; medicine and physician assistants [96]; medicine and psychology [90]; nursing and medicine [133]; nurse practitioner and dentistry [113]; nurse practitioner and medicine [146]; physical therapy and occupational therapy [75, 111]; and psychology interns and primary care physicians [89]. Creating IPP experiences and placements related to service-learning requirements or activities or as a required curriculum course was described in nine articles [58, 67, 74, 91, 97, 101, 110, 115, 121].
Demonstrating educational outcomes through IPP, such as acquisition of competencies related to IPC, discipline-specific competencies (e.g., assessments, interventions, clinical reasoning, etc.), and self-directed learning, was an intention in 26 of the articles [50, 51, 54,55,56, 60, 63, 75, 77, 78, 83, 84, 86, 91, 93, 95, 101, 102, 106, 108, 110, 116, 127, 130, 134, 135]. Gaining knowledge and being able to care for clients from diverse cultural, ethnic, racial, and/or other specific population groups (e.g., children, older adult, vulnerable, etc.) was identified as an intention for 10 of the IPP initiatives [49, 50, 75, 91, 99, 110, 117, 127, 145, 147]. In four articles an intention was to produce reflexive learners and critical thinking in their discipline roles [61, 73, 100, 111], while three aimed to develop interprofessional capacity in primary health care education [52, 108, 116] and five promoted faculty engagement in IPP or collaboration between education and health systems (e.g., academic partnerships) [99, 108, 123, 125, 148]. Developing, piloting, and/or evaluating a model of interprofessional delivery of service was an intention in seven articles [57, 62, 81, 101, 125, 136, 147].
Contributing to the community and creating awareness of the social determinants of health was an intention indicated for 11 of the IPP education initiatives, such as poverty and homelessness [62, 71, 76, 81, 85, 105, 119, 130, 143, 145, 147]. Improving the health care delivery system, addressing gaps in service delivery, addressing the needs of specific communities or populations, and improving care for clients were intentions described in 24 articles [59, 60, 71, 75, 76, 82, 84,85,86, 95, 99, 102, 104, 105, 112, 113, 117, 119, 126, 128, 133, 140, 145, 146], and in five of the articles the goal was production of a skilled workforce that included development of leadership in IPP teams [52, 82, 94, 123, 147]. Increasing the understanding, interest, and number of graduate practitioners in primary health care and rural settings were specific intentions of three IPP education initiatives [94, 108, 130]. Promoting an interprofessional ethos and client-/service user-centered care within a team were also identified as intentions of IPP education initiatives [57, 61, 133]. No explicit intention or purpose for the IPP education initiative was provided in six of the articles; authors in two of these articles refer to previous publications for details on the initiative [53, 66, 68, 90, 129, 132].
Nature of student participation
Nature of student participation reflected how students were involved in the IPP education initiative. For 41 IPP initiatives described in the literature the learning experience was a clinical placement where students of at least one discipline were assigned to participate as part of their educational program with other students from other disciplines participating through elective coursework or volunteerism [49, 53, 55, 56, 59, 62, 63, 68, 74, 77, 81,82,83,84,85,86,87, 93, 95, 96, 98, 103, 104, 106, 107, 109, 111,112,113, 115, 120, 123, 128, 131, 134, 135, 137, 141, 142, 146, 148]. Terms that were considered synonymous with clinical placement included clinical rotation, training site, clerkship, and residency [68, 77, 83, 86, 93, 112, 123]. In seven articles the initiative appeared to be required as part of course work or curriculum for at least one discipline [49, 61, 68, 98, 100, 112, 126] and in 10 instances it appeared to be an elective course or optional experience for credit for at least one discipline [50, 51, 54, 64, 71, 91, 101, 117, 119, 120]. Participation of students in IPP education initiatives was identified as voluntary in 15 articles [52, 60, 66, 69, 79, 97, 108, 114, 118, 122, 125, 127, 132, 138, 145] and three articles suggested either a voluntary nature or clinical practicum requiring an application process [76, 85, 130].
Many articles described a mix of participation models by students from different health disciplines. For example, in seven IPP education initiatives some students could pick either to be volunteers for the initiative or to have a clinical placement at the same initiative [68, 73, 105, 121, 126, 133, 136]. A second model of mixed participation was where some disciplines were mandated to the initiative for clinical practice while other disciplines were there as an elective/optional course or otherwise to receive credit [50, 58, 72, 101, 120, 146]. A third model of mixed participation was where it was voluntary for one discipline but either an elective or receipt of credit for other disciplines depending on program policies [51, 54, 91, 119]. In 19 articles the nature of student participation was either not stated or unclear.
Populations served by the initiative
In addition to a variety of settings where IPP education was situated (Table 1) the initiatives provided services to a range of population groups. By specific age group, services were provided to infants and children [49, 74, 103, 107, 113, 123, 126], adults [70, 81, 136], and older adults (≥60 years old) [50, 57, 66, 83,84,85,86, 105, 112, 116, 117, 146]. Services were provided to patients with specific conditions or disease processes that included chronic disease (e.g., COPD, diabetes, hypertension, HIV, etc.) [51, 53, 57, 59, 62, 65, 78, 80, 81, 92, 95, 111, 118, 121, 132, 141, 148], childhood obesity [73], dementia or cognitive decline [84], disabilities [49, 61, 83, 114], orthopedics [63, 137], and prenatal care [58]. Services were also provided to a mix of age and/or medical conditions, such as: complex and multiple health needs [50, 134]; primary school students and patients with dementia [135]; and varied patient groups or sites associated with an IPP initiative (e.g., diabetes, frail elderly, maternity, nursing homes, palliative care, etc.) [79, 106, 115, 134]. Populations were also defined by specific geographical location that included rural or isolated areas [80, 105, 108, 115, 130, 133, 139, 144, 148], other underserviced or deprived areas [100, 126, 143], and international location [76, 91]. Articles described populations as belonging to a minority, marginalized, vulnerable, uninsured, and/or otherwise socioeconomically disadvantaged group [51, 58, 60, 71, 72, 75, 76, 83, 89, 97, 101, 104, 115, 122, 127, 129, 139, 145, 147], having high utilization of healthcare resources [67], or being veterans [77, 93, 146]. No specific population was identified or clearly stated in 25 articles; however, many of these IPP education initiatives were situated in ambulatory care, primary care, or primary healthcare settings with a general population [77, 79, 89, 94, 98, 100, 102, 115, 125, 138] or residents of facilities, such as long term care [79, 99]. Population was not applicable in one article detailing a practice guide for IPE/IPP [48].
Involvement of instructional personnel and stakeholders
The majority of articles (n = 94) described some aspect of roles and participation of faculty, clinical instructors, site-based professional preceptors or mentors, and/or other stakeholders in the planning and operation of IPP education initiatives. There was variation in terminology used to describe instructional personnel participating from academic settings (e.g., academic educators, academic staff, clinical instructors, clinical supervisors, faculty members, lecturers, practice-educators, professors, university clinical facilitators, residents, teachers) [52, 61, 91, 94, 101, 103, 116, 123, 129, 131, 136, 140, 144, 148] and general use of terms to denote professional positions (e.g., facilitator, mentor, licensed clinicians, nurse educator, placement practitioner, preceptor, primary care preceptor, professional staff) [48, 56, 58, 61, 87, 89, 128, 135, 141], which made it challenging to distinguish whether instructional personnel were strictly from academic institutions or from the host setting. However, professional input to planning and oversight by licensed practitioners, whether from academic or host institutions, was a foundational element in supporting learning of pre-licensure students in IPP education initiatives.
Instructional personnel were involved in planning and coordination of IPP education initiatives that included collaborating on setting goals and objectives, developing activities, identifying community health needs, training practice educators, and setting policies for courses [48, 51, 52, 65, 74, 78, 92, 115]. Stakeholder involvement (e.g., administrators, health insurance planner, policy makers, staff, teachers) from the healthcare setting, service organizations, and other departments included participation in advisory boards, coordination of placements, leadership of clinical education, orientation, pursuit of research initiatives, and the public policy process [64, 74, 81, 95, 99, 102, 114, 129, 147, 148]. Instructional personnel provided or led seminars, educational support, reflective sessions, IP team meetings, reviewed assignments, and other non-clinical teaching activities [98, 101, 112, 118, 131, 140, 141]. Professional oversight of students in placements that was explicitly described was either solely by academic personnel [50, 52, 54, 57, 60, 62, 66, 76, 77, 83, 85, 88, 94, 103, 115, 120, 126, 127, 131, 136, 142, 146, 147] or with involvement of licensed personnel from the healthcare setting [51, 53, 56, 58, 59, 61, 63,64,65, 68,69,70, 72, 75, 82, 86, 87, 89,90,91, 97,98,99, 104, 106,107,108, 110,111,112, 114, 121, 122, 129, 130, 132,133,134,135, 137, 139, 141, 143, 144]. An interprofessional mix of disciplines for instructional personnel in program planning and experiences in clinical settings was clearly noted in much of the literature [51, 53, 54, 58, 59, 63, 66, 68, 74,75,76, 78, 81, 83, 88, 89, 101, 103, 110, 116, 125, 127, 133,134,135,136,137, 142, 146].
There were references to healthcare positions (e.g., clinical coordinator, community practitioner, health care assistant, health education coordinator, health worker, facilitator, IPE facilitator, laboratory staff, supervisor, teaching registrar, tutors) with direct involvement with students but whose professional credentials were unclear [49, 55, 56, 70, 73, 80, 87, 109, 111, 127, 130, 131, 134, 141, 143, 148]. The literature also highlighted involvement of other academic staff and stakeholder personnel, such as support staff (e.g., patient registration specialists, medical assistants, schedulers, etc.) [53, 59, 125, 126], project managers and administrators [102, 108], interpreters or translators [60, 72, 127], lay health promoters [60], teachers or teaching assistants [74, 119], and volunteers [60]. A few articles described IPC and IPP teaching with respect to experience and commitment of instructional personnel, particularly in placement sites, and recommendations were made related to preparation of instructional personnel to support IPP education initiatives [48, 56, 104, 108, 115, 134]. Anderson et al. provides a guide that “…offers a method for engaging clinical frontline practitioners in learning with, and from learners.” (p. 433) for practice-based IPE [48].
Part 3: implementation and Evaluation of IPP Education Initiatives
This section details findings related to: 1) theories, frameworks, and models used in the design of IPP education; 2) teaching and learning strategies used in IPP education initiatives; and 3) evaluation of IPP EL.
Theories, frameworks, and models used to inform IPP education
Authors explicitly referred to using a theory, framework, or model to guide their approach in developing the IPP education initiative in 43 of the included articles (see Table 2). More than one theory, framework, and/or model was used to inform the educational approach in five articles [51, 57, 80, 117, 118]. Of these 43 articles, approximately 63% (n=27) were specific to education and behaviour. Eight articles used a theoretical framework and/or model for EL; two were based specifically on KELT [57, 146] and six were based on the Leicester Model that used Kolb’s work as a foundation [48, 61, 65, 100, 129, 131]. The application of a theory, model, or framework to support IPP education in six other articles was less clear as: a) the underpinnings were not explicitly stated; b) there was scant description of the application of stated theory or model directly to the educational approach (e.g., possibly linked to care delivery model); and/or c) it was difficult to distinguish whether the theory or framework was intended to guide the research approach rather than the educational initiative [60, 84, 97, 122, 130, 135]. There was no indication of a framework or theory to guide IPP education in 44 articles.
Teaching and learning strategies used in IPP education initiatives
A variety of approaches were used to facilitate the IPP education initiatives that were identified in this review. We broadly characterized these approaches as: a) prerequisite and/or corequisite preparation; b) specific teaching and learning strategies; and c) time engaged in the IPP education initiative.
-
a.
Prerequisite and/or corequisite preparation. Prerequisite preparation was characterized by a variety of activities that students were required to complete prior to engaging in the IPP education initiative. Prerequisite preparation was reported in 42 articles. This preparation was delivered through various modes such as: online courses and learning modules [53, 56, 59, 73, 74, 85, 118, 142]; in-person seminars, workshops, and meetings [49, 52, 55, 60, 64, 70, 72, 73, 75, 76, 82, 85, 88, 91, 99, 101, 106, 108, 110, 113, 123, 126,127,128,129, 136, 142, 145]; and individual readings and workbooks [64, 82, 90, 107, 118, 129]. The prerequisite training addressed a variety of topics including an introduction to interprofessional education or interprofessional collaborative practice [53, 56, 59, 60, 72, 76, 83, 99, 101, 103, 108, 113, 118, 123, 142], team building exercises [55, 76, 101, 102, 108, 118], and role expectations of students [52, 83, 99, 103, 118, 126]. Additionally, student orientation to the practice site was commonly a focus of the preparation [49, 52, 59, 64, 70, 76, 83, 85, 90, 108, 126, 145].
Corequisite preparation included some type of complementary learning activity that students were required to engage in at the same time as the IPP experience. Seven of the articles reported a corequisite component to the IPP education initiative [77, 87, 102, 106, 122, 133, 147]. For instance, entire courses or learning modules were intentionally developed and integrated throughout the initiative to complement the clinical experience [77, 87, 102, 133]. These were delivered in-person or online [102, 133], with a focus on such things as: interprofessional roles and responsibilities; effective communication and collaboration; case-based scenarios pertaining to the clinical site; behavioral change and leadership; and, service-learning more broadly [87, 122, 133, 147].
-
b.
Specific teaching and learning strategies. Specific teaching and learning strategies included a wide range of methods and activities to facilitate student participation and support students through the learning process. A variety of specific teaching and learning strategies were presented within the IPP education initiatives included in this review. Having students intentionally work together in small interdisciplinary teams was explicitly reported in 62 of the articles. Teams varied in size, for example, from pairs [49, 56, 58, 59, 63, 65, 68, 108, 128, 137] to groups of three to seven students [70, 76, 78, 79, 85,86,87, 100, 102, 106, 115, 116, 121, 129, 140, 148, 149].
Throughout the experience, students engaged in various activities to facilitate IPP learning. Sixteen of the articles described implementing some type of intentional group discussion to start the day. For instance, team meetings [66, 102, 123], huddles [51, 53, 59, 81, 90, 94, 98, 102], and case conferences [146] were used to organize student groups, allocate client assignments, establish roles and responsibilities, and plan care. A variety of strategies in which students engaged with clients were also reported in 86 of the articles. For instance, students conducted assessments and developed care plans [51, 53, 55, 59, 67,68,69,70, 79, 84, 88, 99, 103,104,105,106, 112, 114,115,116,117,118, 123, 128, 131, 132, 136, 145, 148], delivered direct provision of care and services [50, 58, 63, 76, 78, 80, 81, 102, 107, 109, 120, 122, 126, 127, 134, 137, 141, 142, 146], provided home visits [49, 65,66,67, 86, 90, 98, 112, 117, 131, 140], developed and delivered health promotion or public health intervention or other education [52, 59, 72, 74, 85, 97, 101, 111, 119, 121, 147], engaged in outreach and other service activities [73, 75, 110], actively observed and shadowed healthcare professionals [55, 64, 90, 99, 138], engaged in team meetings or hub discussions [77, 78, 81, 82, 98, 115, 148], and delivered presentations to faculty and stakeholders [67, 77, 88, 93, 96, 105, 108, 111, 113, 115, 127, 130]. Debrief sessions or team meetings at the end of the day to discuss challenges, opportunities, and summarize the day’s experience were reported in 21 of the articles [51, 52, 57, 65,66,67, 70, 71, 76, 78, 81, 86, 92, 98, 102, 108, 110, 113, 118, 125, 128]. In addition, 23 of the articles explicitly reported the use of reflective activities to further help students process their responses to and learnings from the experience [57, 61, 63, 65, 71, 77, 78, 83, 87, 101, 106, 108, 110, 112, 115, 117, 118, 131, 134, 136, 139, 140, 145].
Unique strategies to promote team building throughout the educational experience were noted in five of the articles [85, 113, 126, 137, 144]. These included having shared accommodations, traveling together to the clinical site, and engaging in meals together as strategies for students and faculty to get to know one another, plan for the healthcare initiative, and engage in discussion before and after the day.
-
c.
Time engaged in the IPP education initiative. The amount of time that students engaged in the IPP education initiative was reported in 76 of the articles. However, there was vast inconsistency in the way this was reported and a wide range of timeframes that were noted. For instance, some articles outlined the specific number of hours and/or days per week that students were engaged in the initiative [51, 54, 84, 103, 127] while others reported the overall length of the IPP initiative with little or no additional detail [49, 61, 62, 65, 75,76,77, 80, 96, 98, 99, 101, 106, 111, 113, 115,116,117,118,119, 129, 130, 134, 141, 148]. Overall, the experiences reflected a wide range of timeframes. For example, students may have engaged in a few hours or days [58, 64, 66, 78, 100, 104, 118, 121, 126, 127, 129, 131, 145, 146] up to multiple sessions over a number of weeks [49, 50, 65, 68, 75, 80, 92, 99, 102, 103, 117, 140]. Additionally, the length of engagement for different disciplines within a specific initiative often varied owing to variations in schedules between the departments [51, 53, 55, 59, 81,82,83,84,85,86, 93, 98, 105, 107, 109, 128, 133, 142,143,144].
Evaluation of IPP experiential learning
A range of perspectives and outcomes related to the experiential education initiatives were evaluated and presented in the literature. We broadly categorized these as: a) evaluation of student learning outcomes; b) evaluation of IPP education initiatives; and c) other evaluated outcomes. Various methods and approaches to evaluating and measuring a range of perspectives, learning outcomes, and the impacts of programs were described in the literature, particularly in the articles that reflected either primary research or program evaluation. As such, there were a number of articles that used methods and tools that crossed more than one of the aforementioned categories. For instance, Gruss and Hasnain used a mixed-methods approach to program evaluation that used the Interprofessional Education Collaborative Competency Self Efficacy Tool (IPECC-SET) to evaluate student learning outcomes related to IPC competency development and qualitative responses from students on the benefits of the IPP education initiative [117].
-
a.
Evaluation of student learning outcomes. Dimensions of student learning and professional growth were evaluated and reported in 35 articles. For instance, learning outcomes that were evaluated included competency development, acquisition of specific knowledge and skills, and performance of students who participated in IPP initiatives [50, 51, 57, 86, 98, 99, 108, 113, 114, 116, 117, 123, 126, 130]. Student perceptions and attitudes specific to IPE/IPC/IPP were also evaluated and included views of interdisciplinary practice, learning about interprofessionalism, and appreciation of own and other professional roles [49,50,51,52, 73, 77, 78, 85, 98, 118, 121, 125, 139, 145]. Similarly, perceptions of both students and stakeholders (e.g., preceptors or other involved clinicians) on IPE or IPP were measured [63, 108, 118]. Beliefs and attitudes towards IPP and collaboration were also evaluated [51, 54, 74, 83, 91, 108, 117, 118, 134], as were perceptions about interprofessional teamwork and the experience of workplace learning [51, 57, 79, 136]. Authors also reported changes of awareness and attitudes of students towards clients, the health care system, and care delivery while participating in IPP initiatives [99, 102, 105, 118].
There was a wide range of different tools and methods to evaluate student outcomes related to learning, competency development, perceptions of IPE/IPC/IPP, and other dimensions of their educational experience. The focus of evaluation and corresponding tools or methods used for evaluation are listed in Table 3.
-
b.
Evaluation of IPP education initiatives. Evaluation of the IPP education initiative was reported in 32 of the articles and 15 of these were explicitly described as pilot studies [52, 62, 73, 74, 83, 87, 107, 108, 114, 125,126,127, 130, 133, 140]. The focus of evaluation was categorized into four main themes: a) perceptions of, and attitudes towards, the IPP experience and/or clinical experience; b) description and/or impact of learning in relation to the IPP education initiative; c) perceived value of the IPP education initiative and/or learning from it; and d) evaluation of design, components, instruction, and strategies of the IPP education initiative. The focus of evaluation and corresponding tools or methods used for evaluation or understanding of IPP education initiatives are listed in Table 4. The majority of articles identified as program evaluation used more than one scale and/or other method for evaluation [50, 75, 94, 117, 118, 123, 124, 128]; however, one study used only a survey of student’s experience of the practicum to evaluate the IPP education initiative [56]. One other study evaluated the perceptions of students towards IPE using the Interdisciplinary Education Perception Scale [52].
-
c.
Other evaluated outcomes. Of note, there were other evaluative parameters reported that were not specific to EL but were related to either students’ roles in the services provided and/or tangential outcomes of the IPP education initiative. These included elements, such as client satisfaction in receipt of care, client perceptions of students, client health outcomes related to care through the IPP education initiative, stakeholder (e.g., preceptors, clinicians, agency representatives) perceptions of IPE/IPC/IPP, and other parameters [50, 53, 57,58,59, 61,62,63,64, 84, 93, 94, 101, 105, 107, 118, 128, 129, 131,132,133, 146, 148].


